Severe lower back pain is a common reason people seek medical care, and most cases arise from strains, degenerative changes, or nonspecific causes. However, there is a rare but important possibility that the pain signals cauda equina syndrome (CES), a condition in which the nerves at the end of the spinal cord are compressed. Recognizing the difference between everyday pain and urgent signs may protect bowel and bladder function and preserve mobility. This article outlines the key red flags, practical home steps, what to expect from an evaluation, and common questions people ask.
By understanding when to act promptly and how clinicians approach suspected CES, you can navigate a difficult moment with clear actions. The guidance here emphasizes practical steps you can take today, how to communicate symptoms to a clinician, and what to expect during evaluation and treatment. If you ever notice red flags, seek professional assessment without delay. Remember that online information is not a substitute for in-person care and that a clinician can provide individualized advice.

Red flags: when to seek medical care

Cauda equina syndrome is a medical emergency. If you notice saddle anesthesia, sudden bladder or bowel changes, or rapidly progressive weakness, seek urgent medical care immediately.
Cauda equina syndrome occurs when the nerve roots at the bottom of the spinal cord are compressed. In many cases, back pain arises from common causes, but certain signs may indicate CES and require urgent evaluation. The signs below are red flags to watch for, because they may herald nerve involvement that is time-sensitive:
Saddle anesthesia or numbness in the buttocks, inner thighs, groin, or perineal area; new or worsening difficulty starting or stopping urine, urinary retention, or a sudden change in bladder sensation; new loss of bowel control or incontinence; rapidly developing weakness or numbness in the legs, especially if it makes walking or standing difficult; severe back pain accompanied by numbness or weakness in both legs; a recent injury with worsening neurologic symptoms. If any of these are present, do not delay contact with a clinician or emergency services.
Act promptly. If you notice any of these signs, do not delay care; call emergency services or go to the nearest emergency department.
What may help at home (safely)
At-home steps may support comfort and function while you arrange medical evaluation, but they do not replace urgent assessment if red flags are present.
For many people, conservative strategies can provide temporary relief and keep you mobile while you seek professional advice. Focus on safety and avoiding activities that worsen symptoms. Consider these general approaches if there are no red flags, and you have medical clearance to manage pain at home:
Find a comfortable position that reduces pressure on the spine, and avoid heavy lifting or twisting movements. Gentle walking and controlled daytime movement can help maintain circulation and prevent stiffness. Use heat or cold therapy as tolerated, alternating 15 to 20 minutes at a time, and avoid applying heat over areas with numbness or diminished sensation. Stay hydrated, maintain regular sleep with supportive positioning, and follow label directions if you choose over-the-counter pain relief, while avoiding long-term self-treatment without clinician guidance. Track how symptoms evolve and be prepared to discuss this with your clinician at the next visit.
What to expect during an evaluation

In an evaluation, clinicians review how the pain started, how it progresses, and what other symptoms accompany it. The goal is to determine whether ces is possible, what tests are needed, and how to proceed with care in partnership with you.
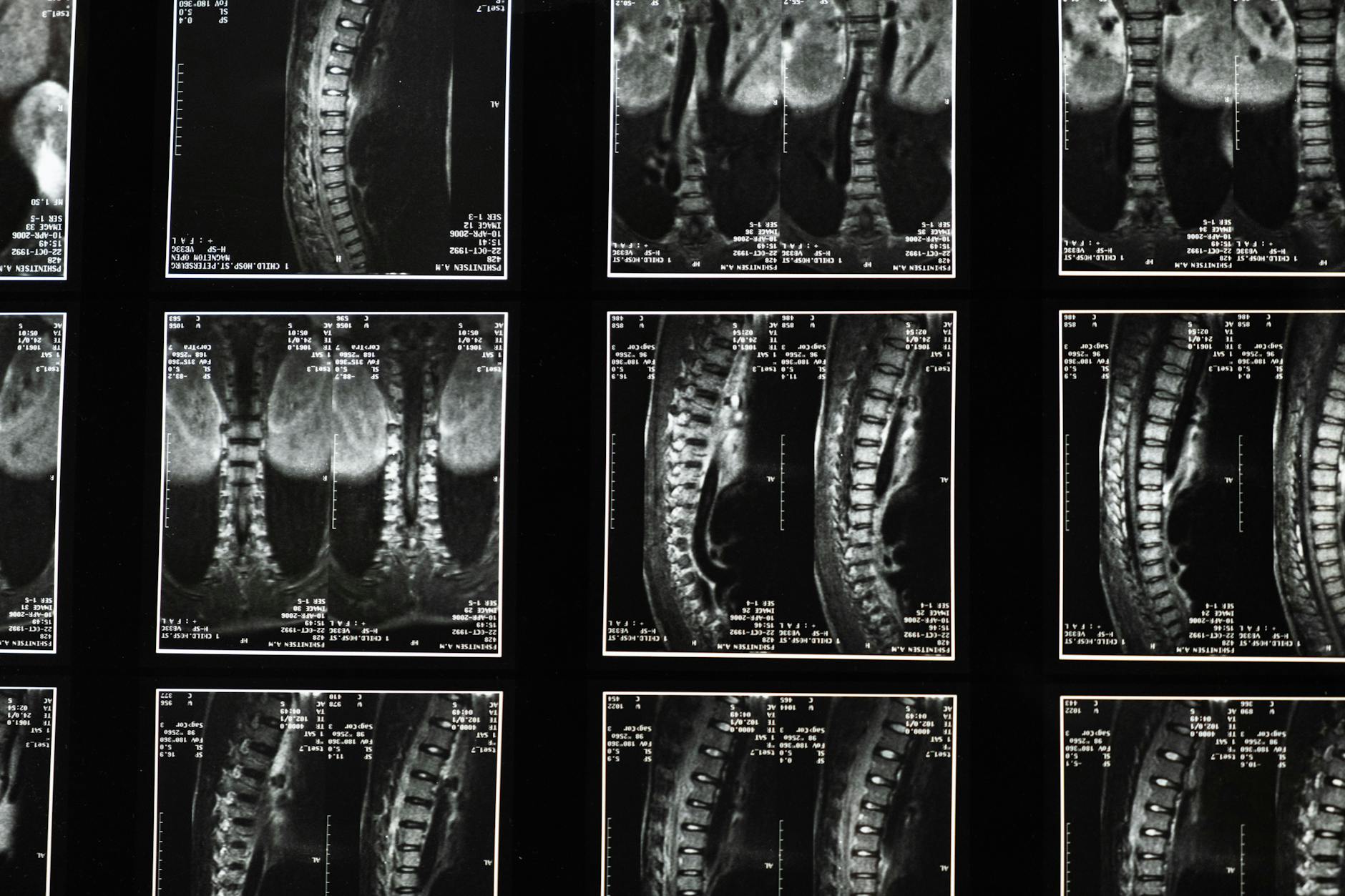
During an evaluation, a clinician will gather a careful history and perform a focused neurologic exam to assess sensation, strength, reflexes, and gait. The clinician will ask about saddle-area symptoms, bladder and bowel changes, and any signs of progression. Depending on findings, imaging—most commonly MRI of the lumbar spine—may be recommended to visualize nerve compression. Blood tests or other studies may be used in specific situations. It is important to recognize the limits of assessment today: a single visit cannot always rule out CES, and decisions are made in collaboration with you, considering symptoms, risks, and preferences.
This process emphasizes shared decision-making, clear communication about what is known and what remains uncertain, and timely steps if CES is suspected. If red flags are present, the path toward urgent imaging and possible admission may be discussed, with safety as the priority. You will be encouraged to ask questions and to express any concerns about treatment options or monitoring plans.
Frequently asked questions

Q: What are the typical signs that CES may be developing?
A: Saddle-area numbness, new or worsening trouble with urination or bowel control, and rapid leg weakness or numbness are among the key signs clinicians monitor. If these occur, seek prompt evaluation.
Q: Is severe back pain always CES?
A: No. Most severe back pain is not CES. CES is a rare but serious emergency, and red flags guide how quickly you should seek care.
Q: Do I need imaging right away?
A: It depends on your symptoms and exam findings. If red flags are present, urgent imaging is often recommended to rule in or out CES; in the absence of red flags, your clinician may take a staged approach based on risk and symptoms.
Q: How should I prepare for an evaluation?
A: Write down when symptoms started, how they progressed, any changes in sensation or function, and current medications. Bring a list of past medical conditions and allergies, and note any red flags you have noticed.
Practical summary
Key takeaways: Severe back pain with new saddle numbness or bladder/bowel changes may signal a serious condition. Prompt evaluation is important, and you have a role in guiding the next steps with your clinician.
- Recognize red flags early and understand why they matter.
- Act quickly by contacting a clinician or emergency services when red flags appear.
- Do not delay evaluation if you notice saddle numbness, bladder changes, or progressive weakness.
- Document onset, progression, and associated symptoms to share with your clinician.
- Prepare a concise medical history and a current list of medications and allergies.
- Ask questions about the need for imaging and the reasoning behind each step in evaluation.
- Follow the clinician’s recommendations for testing, imaging, and monitoring.
- Engage in shared decision-making and implement the agreed-upon care plan with safety in mind.


