Scoliosis in adults versus adolescents presents a mix of shared features and age-specific realities. In teens, scoliosis often appears during growth and may progress as the body changes during puberty. In adults, the curvature can reflect a long-standing condition that evolves more slowly with aging, or it may arise from degenerative changes in the spine. This distinction matters because progression patterns, associated pain, and responses to treatment can differ. By understanding how progression and pain may diverge between these groups, you can approach day-to-day care with clearer expectations and a practical plan for activity, posture, and when to seek professional input.
Across ages, the goal is to support function, minimize discomfort, and preserve quality of life with safe, realistic strategies. This article explains how progression might look in adults compared with adolescents, describes common pain patterns, and offers straightforward, practical guidance for daily life. It also outlines what to expect during an evaluation, how decisions are made in collaboration with a clinician, and which questions are worth bringing to your next visit. The emphasis remains cautious, patient-centered, and grounded in everyday relevance rather than sensational outcomes.
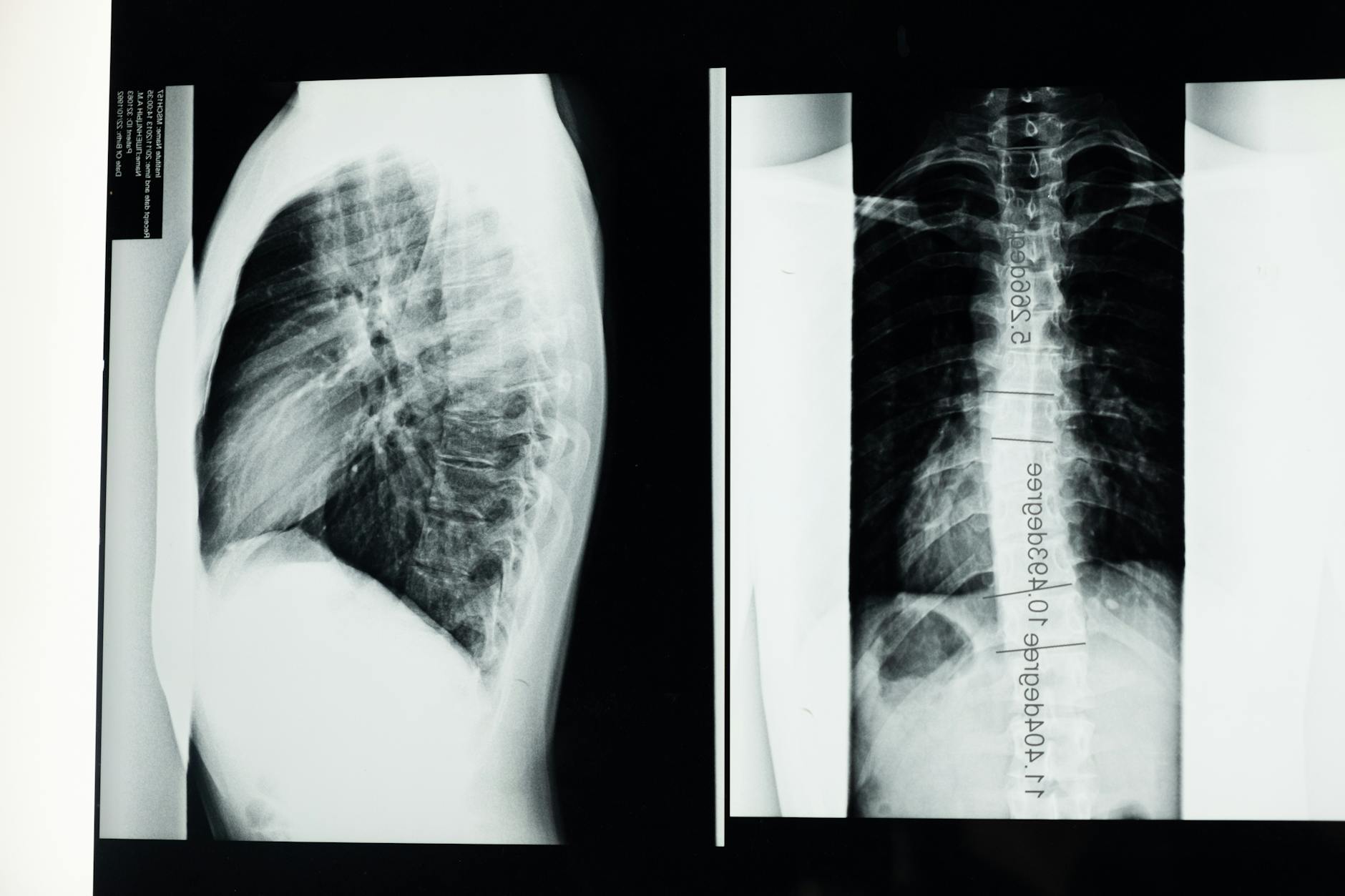
Red flags: when to seek medical care

Most people with scoliosis do not require emergency treatment, but certain signs warrant prompt medical input to rule out other conditions or to adjust a care plan. Adults and adolescents share some concerns, yet the likelihood and implications can differ. If you notice persistent changes in pain, neurological symptoms, or new functional limitations, a careful evaluation can help identify whether the curve is progressing, whether degenerative changes are contributing, or if another issue is present.
Progression in adults often relates to long-term spine changes, while adolescents may experience growth-related shifts that evolve as puberty continues.
- New weakness, numbness, or tingling in the legs
- Difficulty walking or a noticeable change in balance
- Severe, persistent back pain not relieved by rest
- Fever, unexplained weight loss, or night sweats with back pain
- Loss of bowel or bladder control
- Recent major trauma or a fall resulting in worse symptoms
If any of these occur, schedule an evaluation promptly. If the pain is severe, sudden, or accompanied by other alarming signs, seek urgent care. A clinician can determine whether imaging, nerve tests, or other assessments are needed to understand the cause and to tailor a plan tailored to your age, curvature, and lifestyle.
What may help at home (safely)

Self-management components often center on staying active, supporting posture, and aligning daily routines with comfort. For many people, a safe at-home approach can reduce symptoms, improve function, and complement professional care. The emphasis is on consistency, listening to your body, and avoiding positions or activities that worsen pain or difficulty with breathing, walking, or standing.
- Engage in gentle daily movement within your tolerance, such as walking, light cycling, or swimming if comfortable.
- Follow a clinician-approved core and posture exercise program to support spinal alignment and stability.
- Make ergonomic adjustments at work and home to reduce strain on the back and improve posture during daily tasks.
- Incorporate safe stretching and mobility work that avoids painful positions or overextension of the spine.
- Use heat or cold therapy as needed for comfort, while recognizing these are supportive strategies rather than cures.
- Check in with a spine health professional periodically to review progress and adapt your plan as symptoms change.
What to expect during an evaluation
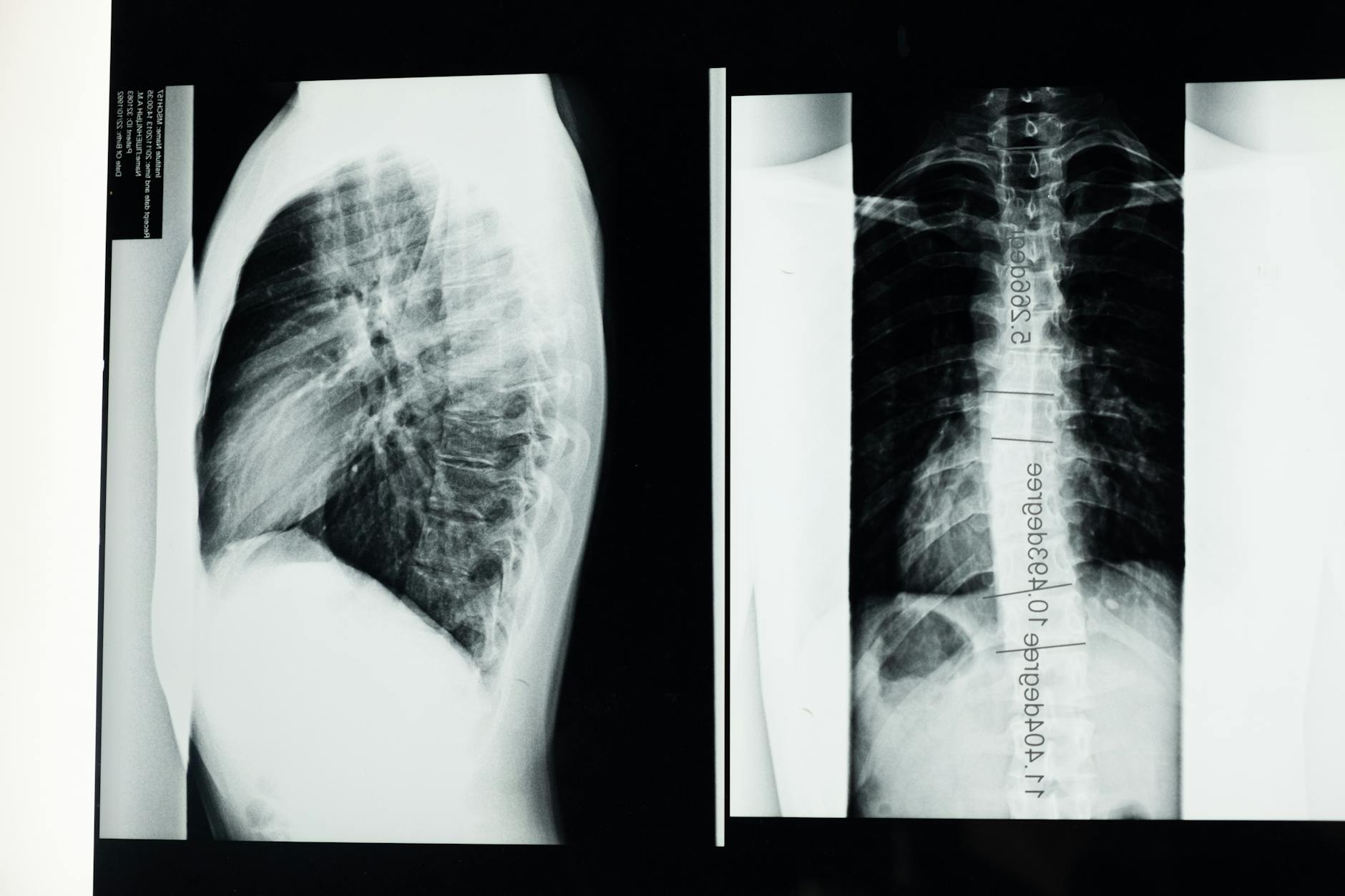
A typical evaluation looks at medical history, current symptoms, functional limits, and how the spine’s curvature affects daily life. A clinician may perform a physical exam to assess posture, flexibility, strength, and balance, and they will review any prior imaging. Imaging may be recommended to better understand the curve and its potential impact on surrounding tissues. The goal is to build a collaborative plan that aligns with your goals, daily activities, and tolerance for risk.
In many cases, management is a shared decision-making process that balances symptoms, function, and personal preferences with reasonable expectations about what can be achieved.
Important nuances include recognizing that not all curves change at the same rate, that symptoms do not always track perfectly with the magnitude of curvature, and that treatment aims to optimize function and comfort rather than achieve a perfect alignment. A clinician can help clarify when to monitor changes, when to pursue targeted therapies such as physical therapy, and which conservative options may be most appropriate before considering more intensive interventions.
Frequently asked questions
Q: Can adult scoliosis progress after adolescence?
A: Yes, progression is possible in adulthood, often related to age-related changes in the spine or to long-standing curvature that gradually evolves. Regular monitoring helps track changes over time.
Q: Are braces useful for adults?
A: Bracing is most often used in growing children, but in some adults, braces may help stabilize symptoms or support posture as part of a broader plan. A clinician can discuss suitability based on your case.
Q: Do exercises or physical therapy change the curve?
A: Exercise programs can improve posture, strength, and pain, and may enhance function. They typically do not reverse the curvature, but they can make daily activities more comfortable.
Q: When should I consider surgery?
A: Surgery is usually considered after conservative options have been explored and there is meaningful, persistent impairment or rapid progression that limits function. This decision is highly individualized and made through careful discussion with your care team.
Practical summary
- Adult and adolescent scoliosis differ in progression patterns and symptom drivers, so management is tailored to age and underlying causes.
- Safe daily activity and posture-focused habits can support comfort and function alongside professional care.
- Early recognition of red flags and prompt medical input help ensure appropriate evaluation and planning.
- Expect a collaborative evaluation process that weighs goals, risks, and practical options for daily life.
- Regular follow-up with a spine health professional helps adjust plans as curves and symptoms evolve.
If you have concerns about scoliosis in adults or adolescents, a personalized assessment with a spine specialist can help you set realistic goals and choose effective next steps aligned with your daily life and preferences.


